Many healthcare patients utilised telemedicine software for the first time during the COVID-19 pandemic, as providers sought to limit access to their physical premises.

To understand more about the uptake of telemedicine and other innovations in healthcare, Capterra surveyed more than 1,000 UK residents who had attended a healthcare appointment within the last 12 months (scroll to the bottom of the article for a full methodology).
In this second article of the series, we explore the issues around data privacy and artificial intelligence (AI) in healthcare and examine the difference in attitudes towards telemedicine among different age groups.
Older patients show more entrenched resistance to telemedicine
88% of telemedicine patients responding to the survey used remote healthcare services for the first time during the COVID-19 pandemic. Most patients (79%) would be happy to continue doing so once the pandemic is over, but a small minority (21%) is more resistant.
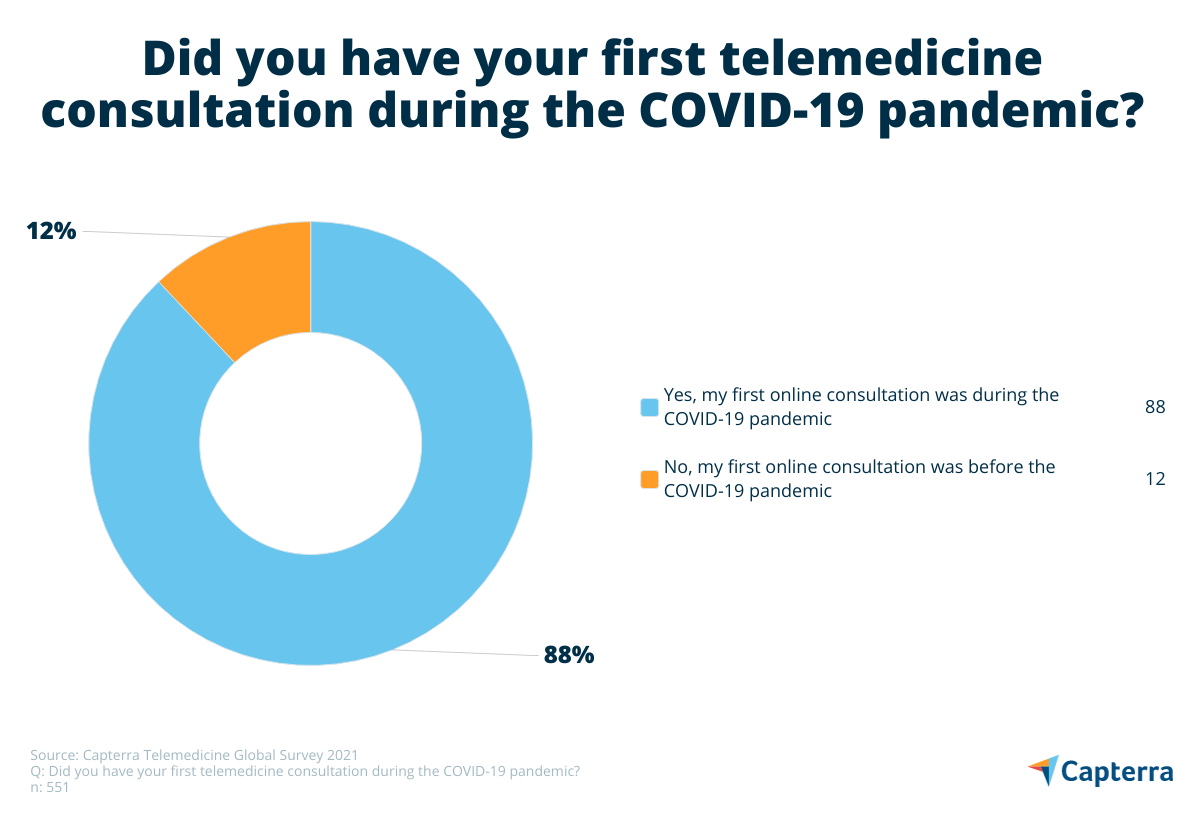
Among the over-65s, the proportion of those who do not want to continue using telemedicine is higher at 43% and overall resistance to telemedicine remains high in this age group. Although there were no major differences in the uptake of telemedicine by different age groups, older patients who had not tried telemedicine were not enthusiastic about doing so in the future. 46% of over-65s in this category say they will always prefer going to a doctor’s office compared with 24% of non-telemedicine-using respondents overall.
82% of telemedicine patients overall say that video consultations will encourage them to consult a doctor online “about the same” (51%) or “more often” (31%). Meanwhile, 40% of over-65s say that they do, or plan to, consult a doctor less often because of the implementation of video consultations.
The provision of remote or virtual services also offers little attraction to this age group. When choosing a new health professional, most age groups would consider one that offers telemedicine (although it wouldn’t be the first criteria). Nearly two-thirds (63%) of over-65s, however, said they don’t make a choice based on this criterion.
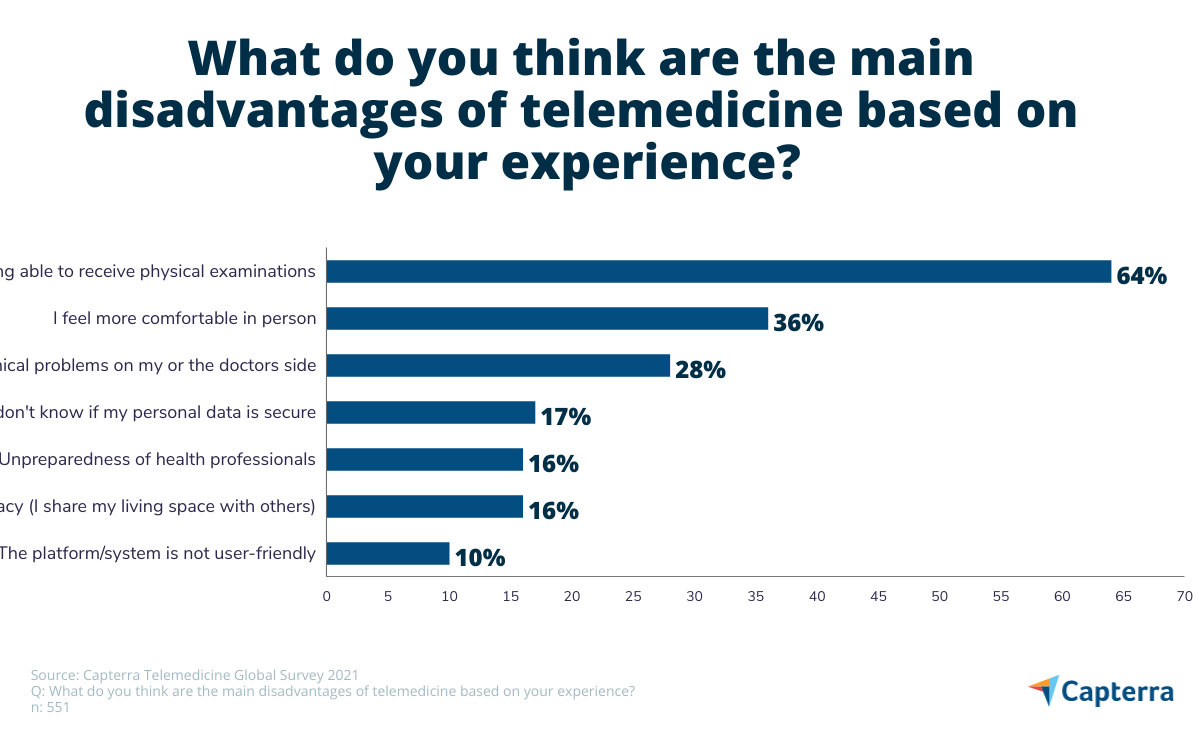
The primary driver of this resistance does not appear to be technophobia or concern about data privacy. Older patients – just like respondents in general – are mainly concerned about not being able to receive a physical examination (41% of over 65s) and say that they feel more comfortable in person (29% of over 65s). They are actually much less concerned about technical issues (7%) compared with telemedicine users in general (28%). The same applies for data privacy concerns (6% versus 17%).
Data privacy not widely understood by telemedicine patients
Using digital health services necessarily involves the transfer and storage of personal and medical data. This raises issues of privacy – a complex subject that not every patient understands well.
Respondents to the Capterra survey showed mixed levels of awareness and concern about how telemedicine providers use the data that patients give.
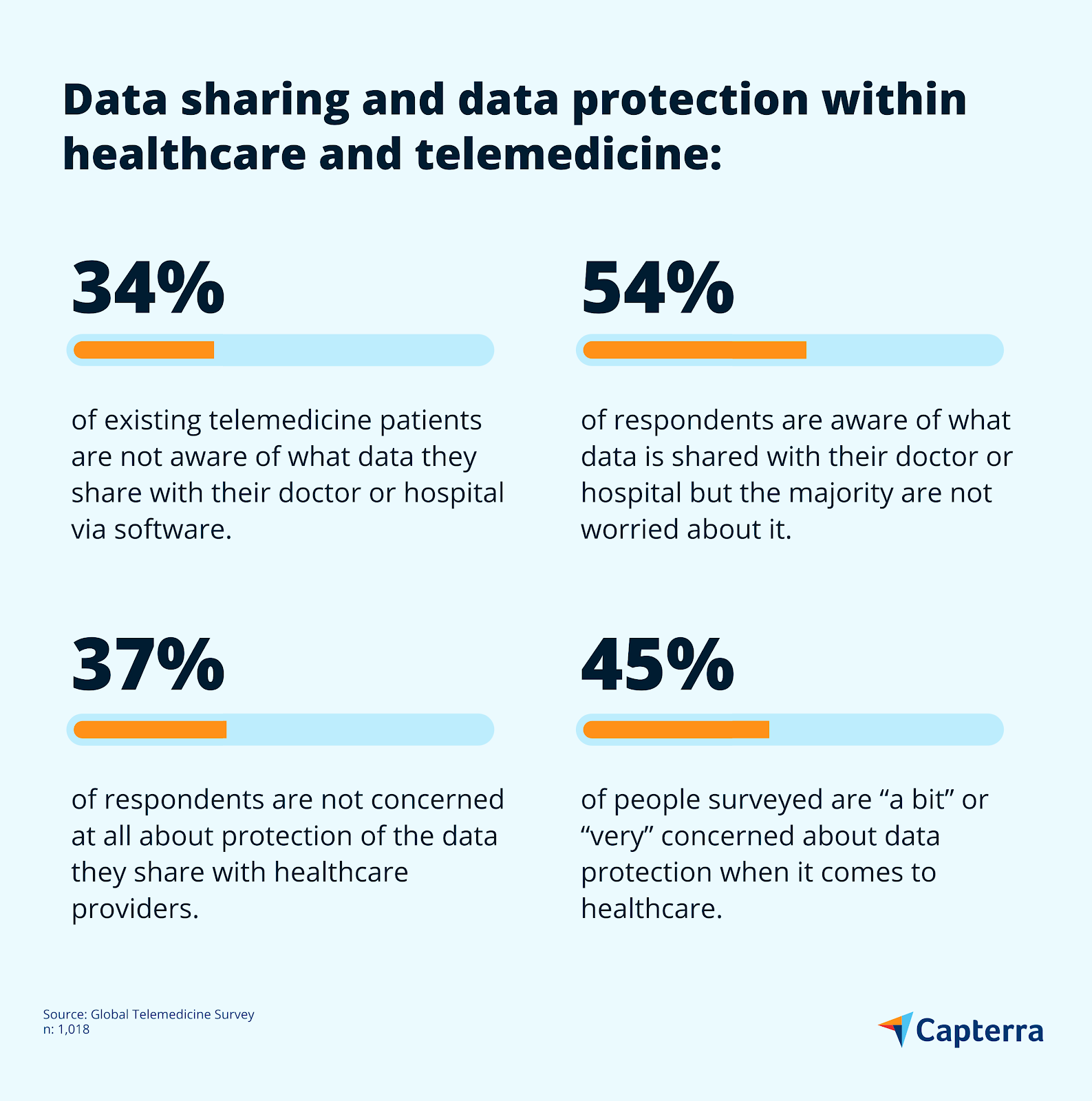
Users of other health apps – such as sleep monitoring or nutrition tracking apps – show similarly mixed awareness and concern about the data they share with the developers of the software. 35% of health app users are aware of how much data they share and are not worried, 26% are aware and worried, while 31% are not aware at all.
Younger respondents to the survey were slightly more aware than their older counterparts about the data they share with healthcare providers and what they do with it. 39% of respondents over the age of 35 were not aware compared with 21% of 18–22-year-olds, for example. And just 2% of over 65s are worried about this issue compared with one-quarter of 23–35-year-olds.
Similar patterns can be found in respondents’ attitudes towards the data they share with healthcare apps such as step counters, sleep trackers, and COVID-19 warning apps.
Although the use of these apps declines sharply with age – 67% of 18–22-year-olds use them compared with 16% of over-65s – older patients are more likely to use COVID-19 warning apps, with 20% of this bracket doing so – the highest of any age group.
Patients are wary of AI-powered medicine
50% of respondents to the Capterra survey think telemedicine is less accurate than face-to-face consultations. But researchers are working to make remote healthcare more effective through artificial intelligence (AI).
Healthcare software has advanced to the point where AI can help doctors diagnose illnesses and propose treatments. Practical applications are not yet widespread in the UK. However, the NHS has an AI lab dedicated to the field, and its own AI report from October 2019 lists several examples:
- Genomics England is exploring how AI can speed up progress in the diagnosis of rare diseases and cancer using data from the 100,000 Genomes Project.
- Doctors are using reports from Mendelian to inform faster diagnosis of rare and hard-to-diagnose conditions.
- BenevolentAI deploys machine learning and AI to accelerate drug discovery and development.
Among respondents overall, 37% are “not sure” what the biggest benefit of AI in health is, but 38% say that it will lead to speedier assistance.
AI is subject to regulations about data privacy – such as the European General Data Protection Regulation (GDPR) – and guidelines regarding medical ethics, such as the UK government’s code of conduct for artificial intelligence (AI) systems used by the NHS.
Overwhelmingly, respondents to the survey are still not convinced about relying on AI for medical treatments or data sharing.
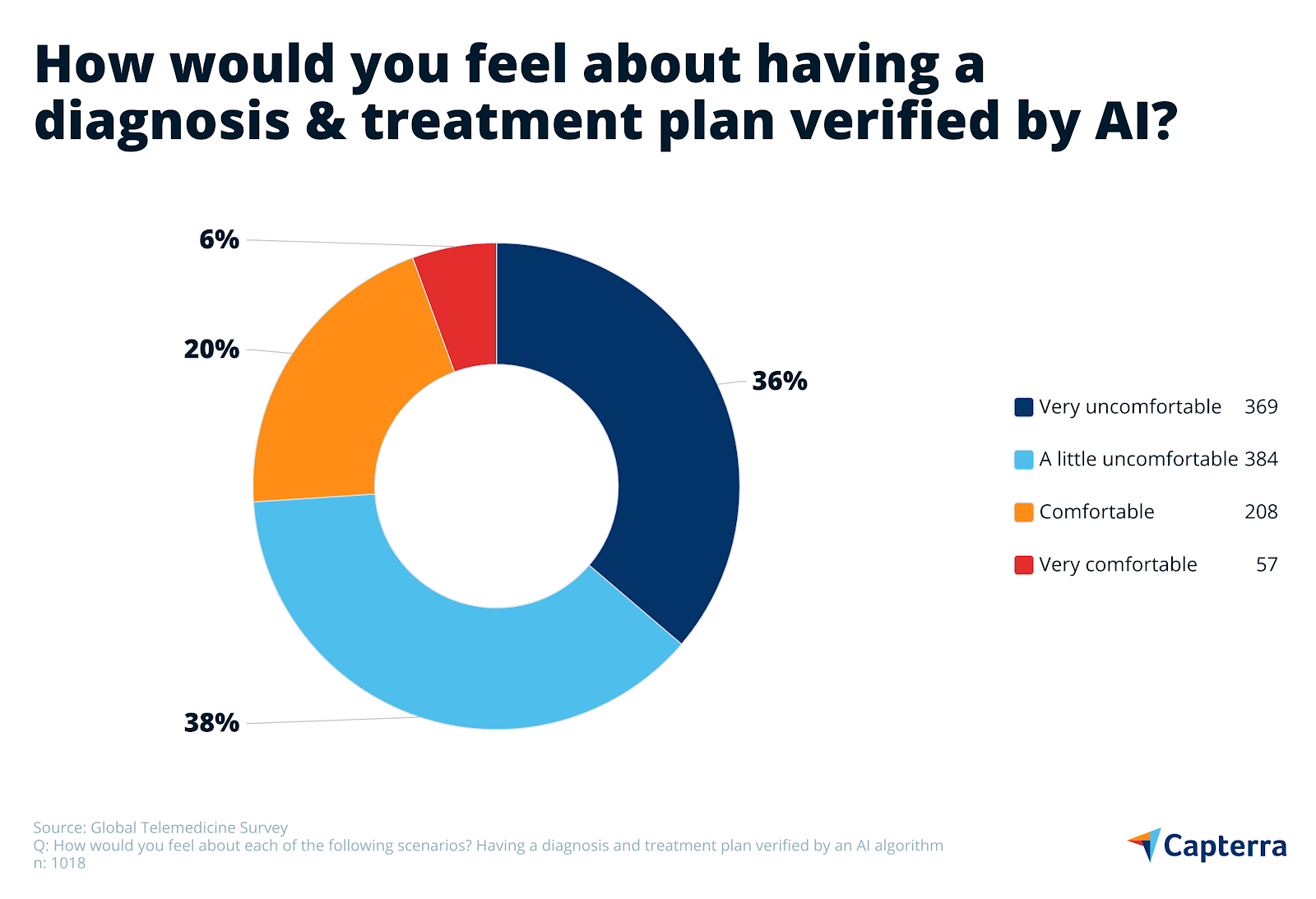
65% of respondents to the Capterra survey would feel uncomfortable with the idea of sharing medical history with an AI-powered virtual assistant before an appointment (24% “very uncomfortable”, 41% “a little uncomfortable”). Similarly, 74% would feel uncomfortable with a diagnosis and treatment plan verified by an AI algorithm (36% “very”, 38% “a little”).
Younger people more open to AI
Younger respondents are more open to the idea of artificial intelligence in healthcare, however. 41% of respondents aged 35 and under would be “comfortable” or “very comfortable” having medication prescribed by AI-powered software, compared with 16% of those aged over 56. And 79% of 35-and-under can name a benefit of using artificial intelligence in health, whereas only 32% of over 65s could do the same.
As AI-powered healthcare applications enter the mainstream, it seems that healthcare providers still have work to do in educating the public about the benefits and risks of the technology.
*Survey methodology
To collect the data for this report, we conducted an online survey in April 2021 Of the total respondents, we were able to identify 1,018 UK respondents that fit within our criteria:
- UK resident
- Over 18 years of age
- Had a healthcare appointment within the last 12 months
- Normally goes to the doctor at least once a year
